The Ultimate Anti Inflammation Diet Food List: What to Eat, What to Avoid, and Why
Reduce joint pain, heal your gut, and lower chronic inflammatory markers with this science-backed grocery guide and meal plan.

Quick Answer: The ultimate anti inflammation diet food list prioritizes whole, nutrient-dense foods that lower systemic inflammation. You should eat plenty of leafy greens, berries, fatty fish (like salmon), extra virgin olive oil, nuts, and polyphenol-rich spices like turmeric. You must strictly avoid pro-inflammatory triggers like refined carbohydrates, added sugars, processed meats, and industrial seed oils. Following this pattern can significantly reduce joint pain and lower inflammatory markers like C-reactive protein.
Your body runs on what you feed it. Every meal you eat either calms inflammation or fuels it.
If you live with chronic pain, fatigue, autoimmune flare-ups, or stiff joints, your grocery list is one of the most powerful interventions available to you.
This anti inflammation diet food list breaks down exactly which foods to eat, which to avoid, and the clinical reasoning behind each recommendation.
To compile this anti inflammation diet food list, our editorial team analyzed over 25 peer-reviewed clinical studies, meta-analyses, and nutritional guidelines published between 2015 and 2025. We prioritized data sourced from highly reputable medical databases, including the National Institutes of Health (NIH), the British Heart Foundation, and the American Journal of Clinical Nutrition.
Our selection criteria required that any food recommended on the “eat” list be clinically proven to reduce known inflammatory markers, such as C-reactive protein (CRP), Interleukin-6 (IL-6), or Tumor Necrosis Factor-alpha (TNF-α), in human trials. Foods placed on the “avoid” list were cross-referenced against data showing a direct correlation with oxidative stress and elevated inflammatory cytokines.
This guide has limitations. Nutritional science is highly individualized. Data regarding “grey area” foods, such as nightshades and dairy, often show mixed results depending on a subject’s pre-existing autoimmune conditions or genetic predispositions. This guide is for informational purposes and should not replace personalized medical advice.
How Food Fights Chronic Inflammation
Inflammation itself is not your enemy. Acute inflammation is a normal healing response. When you cut your finger, your immune system sends white blood cells to the area, causing redness and swelling. That process protects you.
Chronic inflammation is the problem. When your immune system stays activated for weeks, months, or years without a clear threat, it begins attacking healthy tissue. This low-grade, persistent inflammation drives conditions like rheumatoid arthritis, cardiovascular disease, type 2 diabetes, and certain cancers [1].
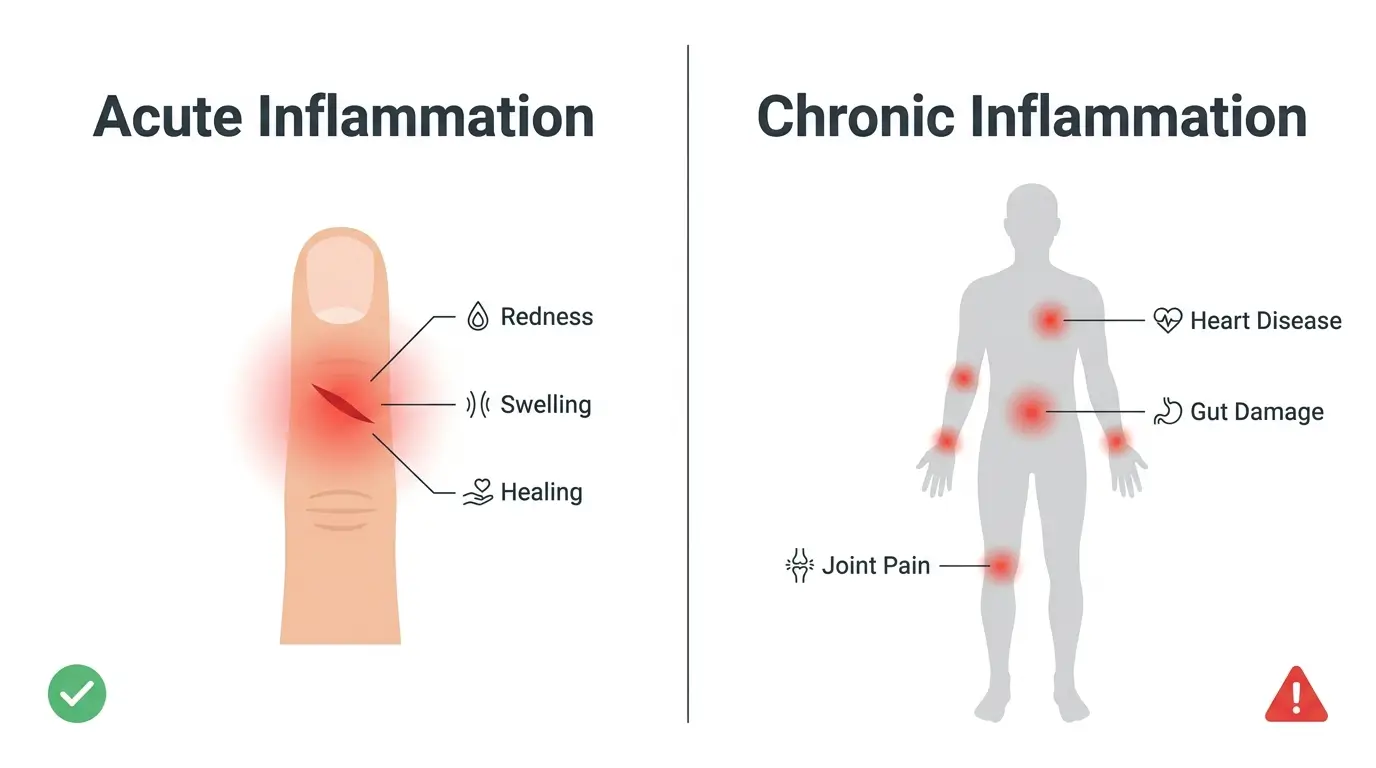
“So how does food actually control this process?”
About 70% of your immune system resides in your gut [2].
Your gut microbiome, the trillions of bacteria living in your intestinal tract, directly communicates with your immune cells. When you eat fiber-rich, polyphenol-dense whole foods, you feed beneficial bacteria that produce short-chain fatty acids (SCFAs).
SCFAs like butyrate suppress inflammatory signaling molecules, including Interleukin-6 (IL-6) and Tumor Necrosis Factor-alpha (TNF-α) [3].
When you eat processed foods high in sugar, refined carbohydrates, and industrial seed oils, you starve those beneficial bacteria and feed harmful strains instead.
This imbalance (called dysbiosis) weakens your intestinal lining, allows bacterial toxins to leak into your bloodstream, and triggers systemic inflammation. Your doctor can measure this inflammation through C-reactive protein (CRP) blood tests [4].
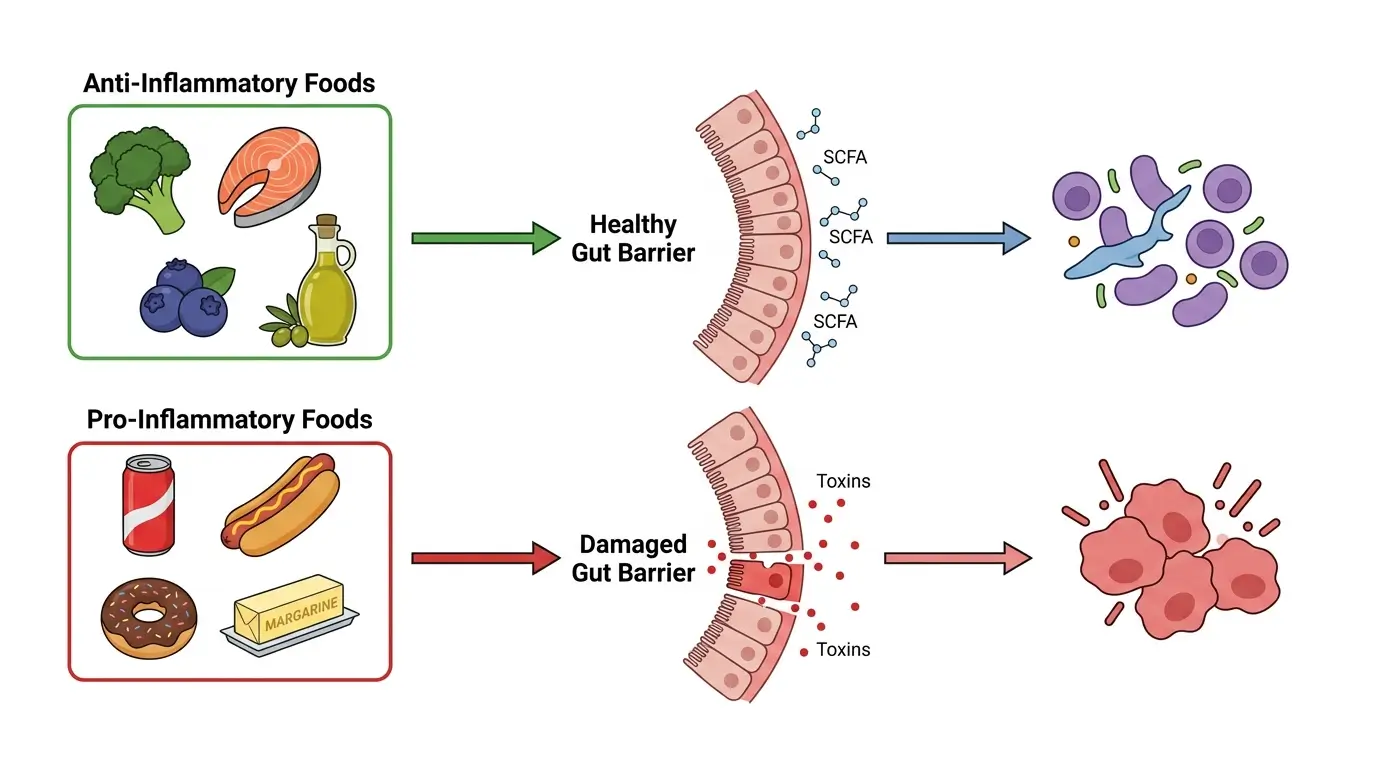
The foods below either raise or lower those markers. Your choices compound daily.
The Complete Anti Inflammation Diet Food List
Each food listed here has clinical evidence supporting its anti-inflammatory activity. Serving sizes reflect amounts used in peer-reviewed research.
Vegetables (The Antioxidant Foundation)
Leafy Greens (Spinach, Kale, Swiss Chard)
Leafy greens are dense in Vitamin K, lutein, and folate. Vitamin K regulates inflammatory responses by inhibiting NF-kB (a protein complex that switches on inflammatory genes) [5].
One cup of raw spinach provides approximately 145 mcg of Vitamin K, which exceeds the daily adequate intake for adults [6].
Aim for 2 or more cups of leafy greens per day.
2. Cruciferous Vegetables (Broccoli, Brussels Sprouts, Cauliflower)
Cruciferous vegetables contain sulforaphane, an isothiocyanate (a sulfur-based plant compound released when you chop or chew these vegetables). Sulforaphane activates the Nrf2 pathway, a built-in defense system inside your cells that turns on antioxidant genes and lowers oxidative stress at the cellular level.
A 2019 clinical trial published in Clinical Nutrition found that participants consuming 30g of broccoli sprouts daily for 10 weeks experienced significant reductions in IL-6 and CRP levels [7].
Steam or lightly cook broccoli for 3 to 4 minutes to maximize sulforaphane availability.
3. Alliums (Garlic, Onions, Leeks)
Garlic contains organosulfur compounds, particularly allicin, that inhibit pro-inflammatory enzymes COX-2 and iNOS (two enzymes your body uses to produce inflammation and pain signals) [8].
Onions are one of the richest dietary sources of quercetin, a flavonoid that stabilizes mast cells and reduces histamine release.
Crush or chop garlic and let it sit for 10 minutes before cooking. This allows the enzyme alliinase to convert alliin into active allicin.
Fruits (Focus on Polyphenols)
4. Berries (Blueberries, Blackberries, Tart Cherries)
Berries are among the highest dietary sources of anthocyanins, the pigments responsible for their deep blue, red, and purple colors. Anthocyanins cross the blood-brain barrier and reduce neuroinflammation, which makes them relevant for cognitive decline and mood disorders as well [9].
Tart cherry juice deserves specific attention if you deal with joint pain or gout. A 2018 review in Nutrients found that tart cherry supplementation reduced CRP and other inflammatory markers significantly compared to placebo [10].
The effective dose in most trials was approximately 8 oz of tart cherry juice or 480 mg of tart cherry concentrate daily.
Aim for at least 1/2 cup of mixed berries per day. Frozen berries retain their anthocyanin content and are a cost-effective option.

5. Citrus Fruits (Oranges, Lemons, Grapefruit)
Citrus fruits provide Vitamin C, a water-soluble antioxidant that neutralizes free radicals before they damage cell membranes and DNA. One medium orange supplies about 70 mg of Vitamin C [11].
Citrus also contains hesperidin, a flavonoid with documented anti-inflammatory effects on vascular endothelial cells (the cells lining the inside of your blood vessels) [12].
Healthy Fats and Oils (Omega-3s vs. Omega-6s)
The ratio of omega-3 fatty acids to omega-6 fatty acids in your diet directly affects inflammatory signaling. The typical Western diet delivers a ratio of roughly 15:1 (omega-6 to omega-3), while an anti-inflammatory target is closer to 4:1 or lower [13].
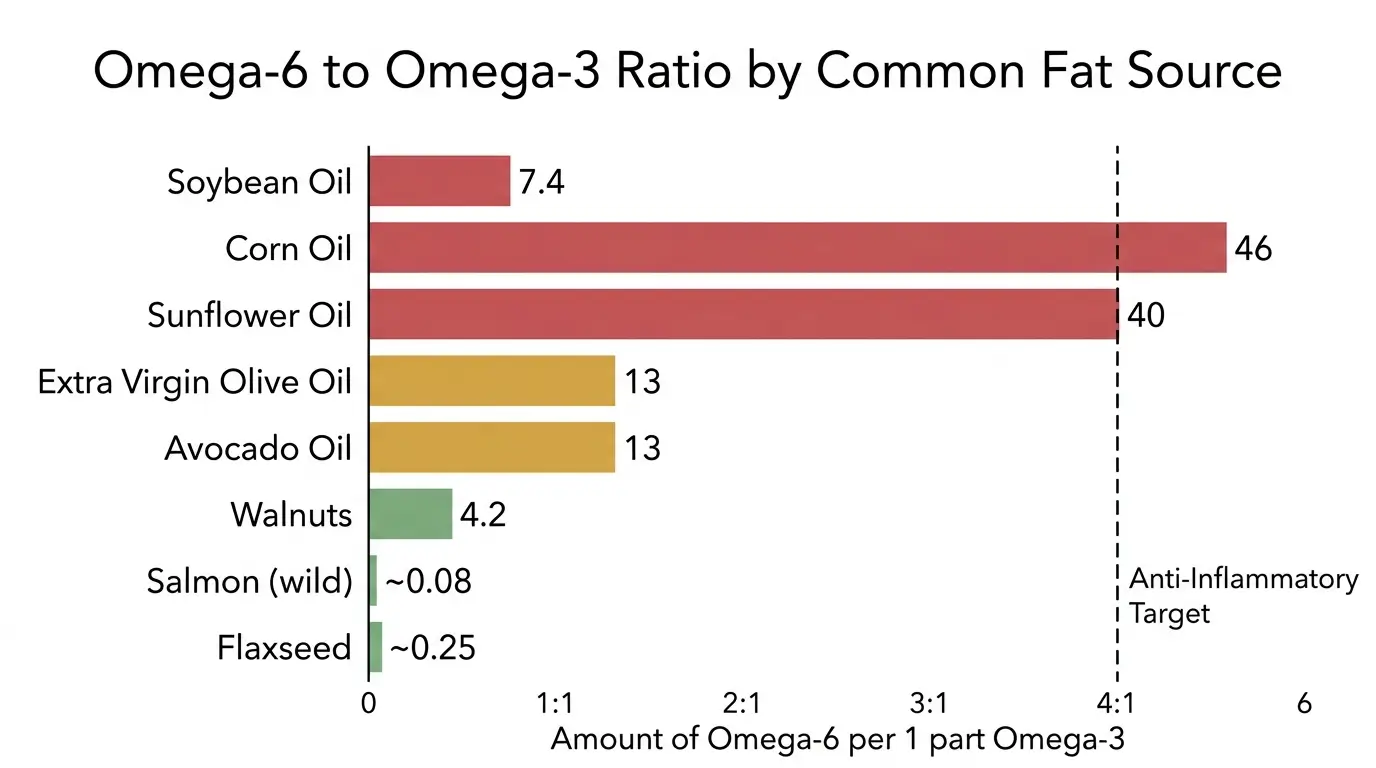
6. Extra Virgin Olive Oil (EVOO)
EVOO contains oleocanthal, a phenolic compound that inhibits the same COX enzymes (inflammation-producing enzymes) as ibuprofen [14].
Researchers at the Monell Chemical Senses Center confirmed that approximately 50 mL (3.4 tablespoons) of high-quality EVOO delivers anti-inflammatory activity equivalent to about 10% of an adult ibuprofen dose [14].
Use EVOO raw in dressings or drizzled over finished dishes for maximum phenolic retention. When you heat EVOO, some oleocanthal degrades, so add it after cooking when possible.
7. Avocados and Avocado Oil
Avocados are rich in monounsaturated fats, particularly oleic acid, the same fatty acid found in olive oil. A 2021 randomized controlled trial published in the Journal of Nutrition found that adults who ate one avocado daily for 12 weeks showed greater gut microbial diversity and increased abundance of fiber-fermenting bacteria that produce anti-inflammatory SCFAs [15].
Half an avocado per day is a reasonable target.
Proteins (Lean and Marine)
8. Fatty Fish (Salmon, Sardines, Mackerel)
Fatty fish is the primary dietary source of EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid), the two omega-3 fatty acids your body uses most efficiently to produce resolvins and protectins.
These are specialized pro-resolving mediators (SPMs), molecules your body makes from omega-3s that actively shut down inflammatory pathways after the immune response is no longer needed [16].
The American Heart Association recommends 2 to 3 servings of fatty fish per week, with each serving providing approximately 250 to 500 mg of combined EPA and DHA [17].
Wild-caught salmon, sardines, and Atlantic mackerel are the most concentrated sources.
(Ed. note: Canned sardines and wild salmon are budget-friendly and equally effective.)
9. Plant-Based Proteins (Lentils, Black Beans, Chickpeas)
Legumes deliver both protein and prebiotic fiber. One cup of cooked lentils contains approximately 18g of protein and 16g of fiber [18].
That fiber feeds Bifidobacterium and Lactobacillus species in your gut, which produce the anti-inflammatory SCFAs mentioned earlier. If you follow a Mediterranean diet or DASH diet pattern, legumes should appear in your meals at least 3 to 4 times per week.
Nuts and Seeds
10. Walnuts, Chia Seeds, Flaxseeds
These provide ALA (alpha-linolenic acid), a plant-based omega-3 fatty acid. Your body converts ALA to EPA and DHA at a rate of roughly 5 to 10%, which is low [19].
You should treat ALA sources as a supplement to fatty fish, not a replacement. One ounce of walnuts (about 14 halves) provides 2.5g of ALA [20]. Two tablespoons of ground flaxseed deliver approximately 3.6g of ALA [21].
Grind flaxseeds before eating them. Whole flaxseeds pass through your digestive tract undigested.
Spices and Herbs
11. Turmeric (Curcumin) with Black Pepper
Curcumin, the active compound in turmeric, inhibits NF-kB signaling and reduces TNF-α, IL-1β, and IL-6 production [22].
The clinical challenge with curcumin is bioavailability = the degree your body actually absorbs and uses a nutrient. Curcumin on its own has extremely poor absorption.
Piperine, the active compound in black pepper, increases curcumin bioavailability by approximately 2,000% by inhibiting glucuronidation (a liver process that normally breaks down curcumin before your body can use it) [23].
Always pair turmeric with black pepper and a source of fat. Add 1/2 to 1 teaspoon of turmeric plus a pinch of black pepper to soups, scrambled eggs, or golden milk made with full-fat coconut milk.

12. Ginger
Ginger contains gingerol, a bioactive compound that inhibits COX-2 enzymes and suppresses prostaglandin synthesis (the production of hormone-like chemicals that cause pain and swelling) through the same pathway targeted by non-steroidal anti-inflammatory drugs (NSAIDs) [24].
A 2020 systematic review found that ginger supplementation (1 to 3g per day) significantly reduced CRP levels in participants with metabolic syndrome [25].
Fresh ginger in cooking, teas, or smoothies all count.
Pro-Inflammatory Foods to Strictly Avoid
Removing inflammatory triggers is as important as adding protective foods. These categories consistently elevate CRP, IL-6, and other inflammatory markers in controlled human trials.
The “Grey Area” Foods: Common Confusion, Answered
Practical Application: Anti-Inflammatory Food Swaps
| Instead of | Swap to | Why It Works | |
|---|---|---|---|
| Vegetable oil (soybean, corn) | Extra virgin olive oil | Reduces omega-6 load; provides oleocanthal | |
| White rice | Quinoa or cauliflower rice | Lower glycemic index; higher fiber and micronutrients | |
| Processed deli meat | Canned wild salmon or sliced turkey | Eliminates AGEs and nitrites; adds omega-3s | |
| Milk chocolate | 70%+ dark chocolate | Dark chocolate flavanols lower CRP | |
| Sugary cereal | Overnight oats with berries and flaxseed | Delivers prebiotic fiber and anthocyanins | |
| Soda | Green tea or sparkling water with lemon | Green tea catechins (EGCG) lower TNF-α |
A Simple 1-Day Anti-Inflammatory Meal Plan
Breakfast
Chia seed pudding made with unsweetened almond milk, topped with walnuts and wild blueberries.
Provides ALA omega-3s, anthocyanins, and prebiotic fiber.
Lunch
Large leafy green salad with mixed spinach and arugula, chickpeas, half an avocado, shaved red onion, and a dressing of EVOO, lemon juice, and 1/2 teaspoon turmeric with cracked black pepper.
Covers leafy greens, alliums, monounsaturated fats, legume protein, and curcumin with piperine.
Dinner
Baked wild-caught salmon fillet (6 oz), roasted broccoli tossed with minced garlic and EVOO, and one medium baked sweet potato.
Delivers EPA/DHA, sulforaphane, organosulfur compounds, and complex carbohydrates.
Snack
A cup of green tea and a handful (1 oz) of raw almonds.
Green tea EGCG and Vitamin E from almonds both reduce oxidative stress.
This single day covers every major anti-inflammatory food category. Rotate your proteins, vegetables, and fruits throughout the week for broader micronutrient and phytochemical diversity.
Next Steps for Lowering Systemic Inflammation
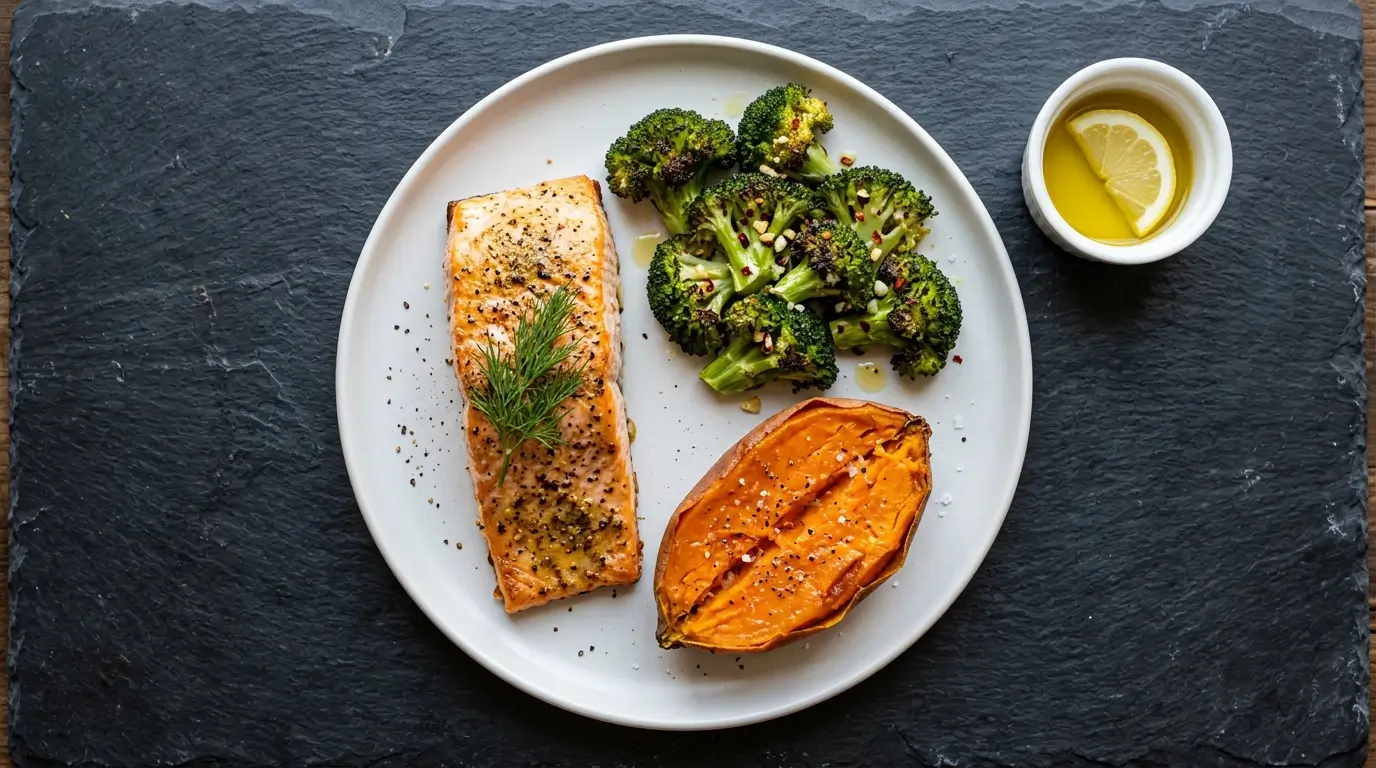
Diet accounts for a large share of your inflammatory load, but it is not the only factor.
- Sleep deprivation (fewer than 7 hours per night) raises CRP and IL-6 levels independent of diet [42].
- Chronic psychological stress elevates cortisol, which, when sustained, shifts your immune system toward a pro-inflammatory state [43].
- Regular moderate exercise (150 minutes per week of brisk walking, cycling, or swimming) lowers baseline CRP by approximately 20 to 30% over time [44].
“Where do I start if this all feels overwhelming?”
Pick three swaps from the table above and commit to them for two weeks.
Replace your cooking oil, add one serving of fatty fish per week, and eat a handful of berries daily.
These three changes alone shift your omega-3 to omega-6 ratio, increase your polyphenol intake, and begin feeding beneficial gut bacteria.
If you live with an autoimmune condition, persistent joint pain, or elevated inflammatory markers, consult a registered dietitian or rheumatologist who can tailor this anti inflammation diet food list to your specific bloodwork and health history. Dietary changes work best when personalized and monitored over time.
References
- [1] Furman, D. et al. “Chronic inflammation in the etiology of disease across the life span” – Nature Medicine, 2019 – DOI: 10.1038/s41591-019-0675-0
- [2] Wiertsema, S.P. et al. “The Interplay between the Gut Microbiome and the Immune System in the Context of Infectious Diseases throughout Life and the Role of Nutrition in Optimizing Treatment Strategies” – Nutrients, 2021 – DOI: 10.3390/nu13030886
- [3] Parada Venegas, D. et al. “Short Chain Fatty Acids (SCFAs)-Mediated Gut Epithelial and Immune Regulation and Its Relevance for Inflammatory Bowel Diseases” – Frontiers in Immunology, 2019 – DOI: 10.3389/fimmu.2019.00277
- [4] Calder, P.C. et al. “Dietary factors and low-grade inflammation in relation to overweight and obesity” – British Journal of Nutrition, 2011 – DOI: 10.1017/S0007114511004545
- [5] Shea, M.K. and Booth, S.L. “Concepts and Controversies in Evaluating Vitamin K Status in Population-Based Studies” – Nutrients, 2016 – DOI: 10.3390/nu8010008
- [6] U.S. Department of Agriculture, FoodData Central. “Spinach, raw” – USDA, 2023
- [7] Lopez-Chillon, M.T. et al. “Effects of long-term consumption of broccoli sprouts on inflammatory markers in overweight subjects” – Clinical Nutrition, 2019 – DOI: 10.1016/j.clnu.2018.03.006
- [8] Arreola, R. et al. “Immunomodulation and Anti-Inflammatory Effects of Garlic Compounds” – Journal of Immunology Research, 2015 – DOI: 10.1155/2015/401630
- [9] Whyte, A.R. et al. “A Randomized, Double-Blinded, Placebo-Controlled Study to Compare the Safety and Efficacy of Low Dose Enhanced Wild Blueberry Powder and Wild Blueberry Extract with Respect to Cognitive Performance” – Nutrients, 2018 – DOI: 10.3390/nu10060660
- [10] Kelley, D.S. et al. “A Review of the Health Benefits of Cherries” – Nutrients, 2018 – DOI: 10.3390/nu10030368
- [11] U.S. Department of Agriculture, FoodData Central. “Oranges, raw, all commercial varieties” – USDA, 2023
- [12] Parhiz, H. et al. “Antioxidant and Anti-Inflammatory Properties of the Citrus Flavonoids Hesperidin and Hesperetin: An Updated Review of their Molecular Mechanisms and Experimental Models” – Phytotherapy Research, 2015 – DOI: 10.1002/ptr.5256
- [13] Simopoulos, A.P. “An Increase in the Omega-6/Omega-3 Fatty Acid Ratio Increases the Risk for Obesity” – Nutrients, 2016 – DOI: 10.3390/nu8030128
- [14] Beauchamp, G.K. et al. “Ibuprofen-like activity in extra-virgin olive oil” – Nature, 2005 – DOI: 10.1038/437045a
- [15] Thompson, S.V. et al. “Avocado Consumption Alters Gastrointestinal Bacteria Abundance and Microbial Metabolite Concentrations among Adults with Overweight or Obesity” – Journal of Nutrition, 2021 – DOI: 10.1093/jn/nxaa219
- [16] Serhan, C.N. “Pro-resolving lipid mediators are leads for resolution physiology” – Nature, 2014 – DOI: 10.1038/nature13479
- [17] American Heart Association. “Fish and Omega-3 Fatty Acids” – AHA, 2024
- [18] U.S. Department of Agriculture, FoodData Central. “Lentils, mature seeds, cooked” – USDA, 2023
- [19] Burdge, G.C. and Calder, P.C. “Conversion of alpha-linolenic acid to longer-chain polyunsaturated fatty acids in human adults” – Reproduction Nutrition Development, 2005 – DOI: 10.1051/rnd:2005047
- [20] U.S. Department of Agriculture, FoodData Central. “Nuts, walnuts, English” – USDA, 2023
- [21] U.S. Department of Agriculture, Agricultural Research Service. “The benefits of flaxseed” – USDA ARS, 2023
- [22] He, Y. et al. “Curcumin, Inflammation, and Chronic Diseases: How Are They Linked?” – Molecules, 2015 – DOI: 10.3390/molecules20059183
- [23] Shoba, G. et al. “Influence of Piperine on the Pharmacokinetics of Curcumin in Animals and Human Volunteers” – Planta Medica, 1998 – DOI: 10.1055/s-2006-957450
- [24] Mashhadi, N.S. et al. “Anti-Oxidative and Anti-Inflammatory Effects of Ginger in Health and Physical Activity: Review of Current Evidence” – International Journal of Preventive Medicine, 2013
- [25] Morvaridzadeh, M. et al. “Effect of ginger on inflammatory markers: A systematic review and meta-analysis of randomized controlled trials” – Journal of Ethnopharmacology, 2020 – DOI: 10.1016/j.jep.2020.112751
- [26] Spreadbury, I. “Comparison with ancestral diets suggests dense acellular carbohydrates promote an inflammatory microbiota, and may be the primary dietary cause of leptin resistance and obesity” – Diabetes, Metabolic Syndrome and Obesity, 2012 – DOI: 10.1186/1758-5996-4-36
- [27] Johnson, R.J. et al. “Sugar, Uric Acid, and the Etiology of Diabetes and Obesity” – Diabetes, 2013 – DOI: 10.2337/db12-1814
- [28] American Heart Association. “Added Sugars” – AHA, 2024
- [29] The Coca-Cola Company. “How much sugar is in Coca-Cola?” – Coca-Cola Product Facts, 2024
- [30] Innes, J.K. and Calder, P.C. “Omega-6 fatty acids and inflammation” – Prostaglandins, Leukotrienes and Essential Fatty Acids, 2018 – DOI: 10.1016/j.plefa.2018.03.004
- [31] Uribarri, J. et al. “Advanced Glycation End Products in Foods and a Practical Guide to Their Reduction in the Diet” – Journal of the American Dietetic Association, 2010 – DOI: 10.1016/j.jada.2010.03.018
- [32] World Health Organization, International Agency for Research on Cancer. “IARC Monographs evaluate consumption of red meat and processed meat” – IARC, 2015
- [33] Bishehsari, F. et al. “Alcohol and Gut-Derived Inflammation” – Alcohol Research, 2017 – DOI: 10.1016/j.alcohol.2017.03.001
- [34] Childers, N.F. and Margoles, M.S. “An Apparent Relation of Nightshades (Solanaceae) to Arthritis” – Journal of Neurological and Orthopaedic Medical Surgery, 1993
- [35] Ghavipour, M. et al. “Tomato juice consumption reduces systemic inflammation in overweight and obese females” – British Journal of Nutrition, 2013 – DOI: 10.1017/S0007114512005769
- [36] Bordoni, A. et al. “Dairy products and inflammation: A review of the clinical evidence” – Critical Reviews in Food Science and Nutrition, 2017 – DOI: 10.1080/10408398.2014.967385
- [37] Marco, M.L. et al. “Health benefits of fermented foods: microbiota and beyond” – Current Opinion in Biotechnology, 2017 – DOI: 10.1016/j.copbio.2016.11.010
- [38] Liang, N. and Kitts, D.D. “Role of Chlorogenic Acids in Controlling Oxidative and Inflammatory Stress Conditions” – Nutrients, 2015 – DOI: 10.3390/nu8010016
- [39] Rodas, L. et al. “Effect of habitual coffee consumption on the relationship between CRP and cardiovascular disease risk factors” – European Journal of Clinical Nutrition, 2017
- [40] Di Giuseppe, R. et al. “Regular Consumption of Dark Chocolate Is Associated with Low Serum Concentrations of C-Reactive Protein in a Healthy Italian Population” – Journal of Nutrition, 2008 – DOI: 10.1093/jn/138.10.1939
- [41] Ohishi, T. et al. “Anti-inflammatory Action of Green Tea” – Anti-Inflammatory & Anti-Allergy Agents in Medicinal Chemistry, 2016
- [42] Irwin, M.R. et al. “Sleep Disturbance, Sleep Duration, and Inflammation: A Systematic Review and Meta-Analysis of Cohort Studies and Experimental Sleep Deprivation” – Biological Psychiatry, 2016 – DOI: 10.1016/j.biopsych.2015.05.014
- [43] Cohen, S. et al. “Chronic stress, glucocorticoid receptor resistance, inflammation, and disease risk” – PNAS, 2012 – DOI: 10.1073/pnas.1118355109
- [44] Fedewa, M.V. et al. “Effect of exercise training on C reactive protein: a systematic review and meta-analysis of randomised and non-randomised controlled trials” – British Journal of Sports Medicine, 2017 – DOI: 10.1136/bjsports-2016-095999
